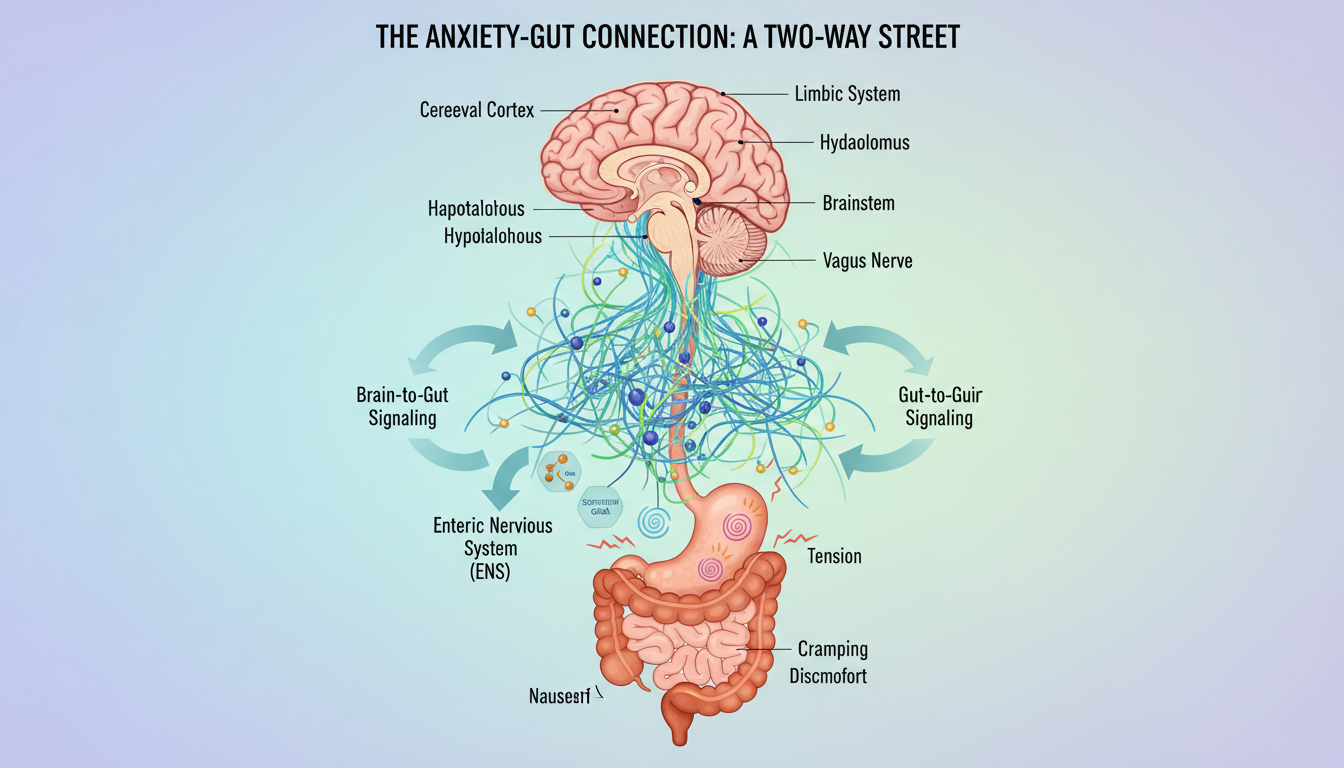
Have you ever felt a knot in your gut during a stressful moment, wondering if it’s all in your head? That physical unease is a real signal from your body.
It represents a tangible manifestation of mental distress. This connection is powerful and affects millions.
These experiences range from temporary butterflies to chronic digestive discomfort. They can significantly impact daily life and overall wellbeing.
Common signs include cramping, nausea, bloating, and changes in bowel habits. These often flare up during periods of high pressure or worry.
Understanding this link between your mind and digestive health is the crucial first step. It paves the way toward finding effective relief and management strategies.
This guide will explore the science behind these reactions. We will provide practical management techniques, dietary adjustments, and guidance on when to seek professional care for stress-related stomach pain.
Please know that these challenges are common and very treatable. Many people successfully manage their condition with the right combination of lifestyle changes and support.
Key Takeaways
- The physical sensations in your gut during stress are real, not imagined.
- Discomfort can vary from short-lived to ongoing, affecting quality of life.
- Typical signs include cramping, nausea, bloating, and altered bowel movements.
- Recognizing the brain-gut link is essential for effective management.
- Actionable strategies based on medical research can provide significant relief.
- These conditions are common, and successful treatment is possible.
- Knowing when to consult a doctor is a key part of taking control.
Understanding Stomach Anxiety Symptoms
The body has a direct line for broadcasting emotional turmoil, and its favorite channel is often the digestive tract. This isn’t imagination. It’s a real physical response to mental strain.
What They Are and Why They Occur
When we feel stressed, our brain releases hormones like cortisol and adrenaline. These chemicals trigger real changes in our gut. The resulting discomfort is a legitimate nervous system reaction.
The Gut-Brain Connection Explained
A major communication highway, the gut-brain axis, links these two areas. The vagus nerve and the enteric nervous system in your GI tract form this two-way street. Signals flow constantly between your head and your belly.
| Common Physical Signals | Typical Descriptors |
|---|---|
| Upper Abdominal Sensation | “Butterflies,” churning, or a knotted feeling |
| Digestive Discomfort | Bloating, excess gas, or cramping |
| Bowel Habit Changes | Sudden diarrhea or constipation |
| Appetite Shift | Loss of appetite or mild nausea |
Recognizing this connection is the vital first step toward managing both the mental and physical aspects of your well-being.
How Anxiety Impacts the Digestive System
The physical unease you feel isn’t random; it’s a precise biological process set in motion by your nervous system. This process affects multiple aspects of your gut’s function.
Hormonal Responses and Stomach Acid
When stressed, our body releases cortisol. This key hormone signals the production of excess acid in the gut.
This acid can irritate the lining of the esophagus and the stomach itself. The result is a burning sensation, nausea, and in persistent cases, even ulcers.
Stress chemicals also alter gut motility. This is the rhythmic squeezing that moves food. It can speed up or slow down, causing diarrhea or constipation.
Furthermore, this strain disrupts the delicate balance of bacteria in our GI tract. An imbalanced microbiome directly contributes to bloating and intestinal pain.
Chronic worry also leads to abdominal tension. Tight muscles in the core region tire easily, creating a cycle of recurring discomfort.
| Anxiety Trigger | Physical Effect | Resulting Sensation |
|---|---|---|
| Hormonal Surge (Cortisol) | Excess Acid Production | Burning pain, nausea |
| Neurotransmitter Release | Altered Gut Motility | Diarrhea or constipation |
| Nervous System Activation | Microbiome Imbalance | Bloating, upset stomach |
| Sustained Muscle Tension | Abdominal Muscle Fatigue | Aching, knotted feeling |
These are the real mechanisms behind anxiety-related indigestion. Understanding them shows why managing stress is crucial for your digestive.
Recognizing the Link Between Anxiety and IBS
When ongoing stress leads to persistent gut issues, it may be more than just temporary discomfort; it could be irritable bowel syndrome. This common digestive condition is strongly tied to our emotional state.
Irritable bowel syndrome, or IBS, involves a digestive system that functions poorly without a clear organic cause. The result is altered bowel movement and abdominal uneasiness.
Identifying Overlapping Symptoms
Many signs overlap between general stress responses and this chronic condition. This makes identification tricky without professional insight.
Shared indicators include constipation, bloating, and diarrhea. Abdominal pain and unpredictable bowel patterns are also common.
| Symptom Type | General Anxiety Response | IBS Flare |
|---|---|---|
| Bowel Habit Change | Occasional, stress-linked | Chronic, unpredictable |
| Abdominal Sensation | Temporary cramping | Persistent pain or discomfort |
| Digestive Distress | Short-lived bloating | Frequent, severe bloating |
For those with existing IBS, worry can trigger major symptom flares. This creates a difficult cycle where digestive troubles increase mental strain, which then worsens the physical condition.
Understanding whether your experiences are temporary or point to a chronic issue like IBS is vital. A proper diagnosis from a gastroenterologist is essential, as treatment paths differ.
Exploring Triggers: Stress, Diet, and Lifestyle
Our modern lifestyles, filled with constant demands and quick meals, often set the stage for physical unease. Effective management begins by pinpointing the specific factors that spark your discomfort.
Common Stressors and Their Effects
Emotional pressures are frequent catalysts. These include job deadlines, relationship strains, financial concerns, and significant life changes.

Chronic strain often disrupts eating patterns. People may skip meals, overeat, or crave sugary comfort foods that upset digestion.
Foods high in natural or artificial sugars are common culprits. They are poorly digested, leading to gas, bloating, and abdominal pain.
Lifestyle habits like smoking, excessive alcohol, and high caffeine intake also irritate the GI tract. They can directly trigger or worsen existing issues.
| Trigger Type | Common Examples | Potential Physical Effect |
|---|---|---|
| Emotional Stress | Work pressure, financial worry | Increased gut sensitivity, cramping |
| Dietary Choice | Sugary snacks, fatty foods | Bloating, gas, stomach discomfort |
| Daily Habit | High caffeine, alcohol use | Acid reflux, intestinal irritation |
Even mild indigestion can amplify feelings of worry. This can create a difficult cycle where slight pain fuels more anxiety.
Identifying your unique triggers is a powerful step. Keeping a simple diary to log meals, daily events, and any discomfort can reveal clear patterns for you to address.
Step-by-Step Strategies for Managing Symptoms
Taking control of your physical reactions begins with simple, actionable steps you can practice daily. These methods help calm your nervous system and ease digestive distress.
Consistency is key. Regular practice teaches your body to shift from a stressed state to a relaxed one more easily.
Deep Breathing and Mindfulness Techniques
Start with focused breathing. Inhale slowly through your nose, letting your belly expand. Exhale fully, feeling your abdomen soften.
Set a reminder to pause for one minute every few hours. This short break can reset your stress levels. It soothes both mind and gut.
Mindfulness meditation builds on this. A body scan helps you notice and release tension held in your core area.
Practical Exercises to Ease Tension
Progressive muscle relaxation targets physical tightness. Systematically tense then release muscle groups, starting with your feet and moving upward.
Pay special attention to your abdominal region. Releasing this tension can reduce associated pain.
Gentle yoga poses also offer relief. Child’s pose and seated twists massage internal organs. They promote better digestion.
| Technique | How to Practice | Primary Benefit |
|---|---|---|
| Diaphragmatic Breathing | Inhale through nose, belly out; exhale slowly. | Activates relaxation response quickly. |
| Body Scan Meditation | Focus awareness from head to toes, releasing tension. | Reduces mental worry and physical holding. |
| Progressive Muscle Relaxation | Tense then relax each muscle group systematically. | Eases overall bodily tension. |
| Gentle Yoga Stretches | Hold poses like child’s pose for 30-60 seconds. | Improves circulation and digestive motility. |
Incorporate these strategies before meals or during known stressful periods. Over time, they become powerful tools for managing your well-being.
Practical Dietary Adjustments for a Calm Gut
Navigating dietary choices is key to managing discomfort from the gut-brain connection. What you eat can either soothe or inflame your digestive system.
Build your diet on a foundation of fruits, vegetables, and whole grains. These support healthy digestion. Water and fresh juices keep you hydrated.
For acute stomach pain, choose plain foods. Try crackers, toast, rice, bananas, or broth. They are gentle and help settle your gut.
If you have stress-related hyperacidity, increase dairy intake. Opt for non-spicy items to soothe your stomach lining. Avoid spicy, fatty, or sugary foods.
These can cause gas, bloating, and indigestion. This discomfort can worsen feelings of anxiety.
Natural remedies like peppermint tea can ease pain and cramping. Also, avoid overeating. A very full stomach can be misinterpreted as pain by your nervous system.
A practical tip is to eat smaller, frequent meals. This pattern minimizes stress on your gut while ensuring good nutrition.
When to Seek Professional Medical Advice
While many gut reactions to stress are temporary, certain signs demand professional medical evaluation. Recognizing these signals is key for your long-term health.
Warning Signs That Need Attention
Specific red flags point to a more serious condition. These include unexplained weight loss, blood in the stool, or black, tarry stools.
Abnormal blood tests that reveal anemia also require a doctor’s attention. Severe abdominal pain with fever or vomiting needs an immediate visit.
Chronic GI issues lasting weeks or recurring often warrant a specialist’s evaluation. A gastroenterologist can perform tests for a precise diagnosis.
We emphasize regular preventive care. See your primary doctor yearly and discuss any ongoing digestive discomfort.
| Concerning Sign | Possible Indication | Recommended Action |
|---|---|---|
| Unexplained Weight Loss | Underlying metabolic or organic disorder | Schedule appointment with primary care physician |
| Blood in Stool | Bleeding in digestive tract | Seek prompt medical evaluation |
| Severe Stomach Pain with Fever | Possible infection or inflammation | Visit doctor or urgent care immediately |
| Chronic Symptoms (weeks) | Irritable bowel syndrome or other conditions | Consult a gastroenterology specialist |
| Recurring Discomfort after Stress | Anxiety-related gut sensitivity | Discuss integrated mind-body treatment options |
Seeking care validates your experience. It ensures the right diagnosis, whether the cause is stress or a physical health issue.
Therapies and Treatments for Digestive Discomfort
Finding relief from digestive discomfort often involves a combination of accessible remedies and expert guidance. A comprehensive treatment plan addresses both immediate sensations and their root causes.
We will explore options ranging from pharmacy shelves to specialist clinics. This approach ensures you have tools for acute episodes and long-term management.
Over-the-Counter and Home Remedies
For sudden flare-ups, several solutions can help. Over-the-counter antacids manage excess acidity, offering temporary respite.
Natural choices like peppermint tea or capsules soothe the intestinal lining. Ginger eases nausea, while chamomile promotes relaxation.
Remember, these treatments calm the gut but don’t resolve underlying stress. They are best used for symptomatic relief during tough moments.
Insights from Gastroenterology Experts
Persistent issues require a professional evaluation. Board-certified experts, like those at Manhattan Gastroenterology, perform thorough assessments.
They rule out other conditions and identify your unique triggers. Together, you build a personalized plan for better health.
If recurring panic attacks cause stomach pain, your doctor may suggest counseling. Working with a therapist using cognitive-behavioral therapy can break the cycle.
The most effective care blends medical management for physical pain with psychological support. This integrated strategy leads to lasting improvement.
Lifestyle Changes to Alleviate Anxiety and Improve Digestion
Simple shifts in your daily routine can powerfully influence your mental state and digestive comfort. Fundamental changes start with regular movement. Avoid sitting for long periods, as this can worsen both mental health and gut function.
Prioritize getting at least seven hours of sleep each night. Sleep deprivation significantly increases feelings of anxiety and disrupts your digestive system.
Exercise and yoga are excellent for reducing stress. Even a few minutes daily helps. Your body releases endorphins that interact with brain receptors, triggering positive feelings.
Protect your mental health by learning to say no. Trying to please everyone creates chronic stress and long-term suffering.
Social connection is vital. Laugh regularly and spend time with supportive people. Many people find that being outdoors in nature greatly reduces anxiety and boosts overall health.
Limit alcohol and caffeine intake, as these can worsen stomach issues. Choose healthy foods that support good digestion.
These changes work together. Combined, they build a strong foundation for managing your well-being more effectively than any single step. For more on managing daily pressure, visit workshiftanxiety.com.
Maintaining Holistic Health: Body and Mind
The most effective care plans address the whole person. They recognize that mental clarity and digestive comfort are deeply linked.
This holistic view treats your brain and gut as one system. Each plays a vital role in your overall health.
Long-term success relies on integrated strategies. These support both psychological resilience and optimal gut function.
Integrating Exercise and Rest
Regular movement is a cornerstone. It clears the mind and promotes healthy digestion.
Equally important is quality sleep. It allows your body to repair and regulate stress hormones.
Balance is key. Too much or too little of either can disrupt your system.
Long-Term Management Techniques
Ongoing communication with your doctor is crucial. Your primary care physician can help reduce stress.
They can also identify signs of a chronic GI condition. A referral to a specialist may be needed.
Don’t hesitate to talk to a therapist or counselor. Sharing your stressors is a powerful tool.
Modern resources like meditation apps make daily practice easy. They offer accessible support for mental health.
| Core Practice | Physical Benefit | Mental Benefit |
|---|---|---|
| Consistent Exercise | Improves gut motility | Boosts mood, reduces worry |
| Adequate Sleep | Allows tissue repair | Regulates emotional response |
| Professional Guidance | Rules out other conditions | Provides structured support |
| Mindfulness Routine | Calms nervous system | Enhances present-moment focus |
The fact is, lasting health comes from consistent changes. It’s not about perfection.
Build a sustainable plan with multiple ways to support this connection. Your body and mind will thank you.
Final Thoughts for a Healthier Stomach
Recognizing the mind-gut link empowers you to take charge of your well-being from both angles. These physical reactions are genuine signals from your body.
They highlight a powerful connection between mental strain and digestive function. For lasting relief, address both areas together.
Do not let stress-related pain limit your life or joy. Many people face these issues, and seeking help is a strength.
A gastroenterologist or therapist can create a personalized care plan for you. With the right strategies, you can feel better and thrive.